A blastocyst is a Day-5 or Day-6 embryo containing a defined inner cell mass (future fetus) and trophectoderm (future placenta). The blastocyst stage offers the highest implantation potential in IVF and allows clearer embryo grading and genetic testing. Guaranteed Blastocyst programs focus on defined embryo outcomes before transfer planning begins.
Forms Day 5–6 after fertilization
Contains ICM + trophectoderm
Highest implantation potential
40–60% reach this stage
Enables structured IVF planning
EggDonors4All provides education and coordination only. All embryo creation, testing, freezing, and transfer procedures are performed by licensed fertility clinics.
A blastocyst is an embryo that has developed for five to six days after fertilization. It represents the first major structural milestone in early human development.
At this stage:
In simple terms:
A blastocyst is the stage at which an embryo becomes organized and ready to implant.
This is why most modern IVF programs prefer transferring embryos at the blastocyst stage rather than earlier (Day-3 cleavage stage).
For detailed terminology, see:

Inner Cell Mass (ICM)
The group of cells that becomes the fetus.
Trophectoderm (TE)
The outer layer that becomes the placenta.
Blastocoel
The fluid-filled cavity that allows expansion.
Zona Pellucida
The protective shell surrounding the embryo, which must be shed (“hatching”) before implantation.
This differentiation between inner and outer cells is what distinguishes a blastocyst from earlier stages like the morula.
Understanding how a blastocyst forms helps clarify why not all embryos reach this stage.
| Stage | Day | Description |
| Zygote | Day 1 | Single fertilized cell |
| Cleavage | Day 2–3 | Rapid cell division |
| Morula | Day 4 | Compact ball of cells |
| Blastocyst | Day 5–6 | Differentiated + expanded |
| Implantation | Day 6–10 | Attaches to uterine lining |
Only about 40–60% of fertilized eggs reach the blastocyst stage.
This percentage varies depending on:
For deeper analysis:
Blastocyst Stage — Complete Overview
The blastocyst stage is critical for four reasons:
Highest Implantation Potential
Blastocysts have passed key developmental checkpoints.
Allows Genetic Testing (PGT-A)
Biopsy is typically performed at the blastocyst stage.
Aligns with Natural Implantation Timing
The uterus is most receptive around Day 6–10.
This is why blastocyst transfer is now the standard in many fertility programs.
Technically:
A blastocyst becomes an implanted embryo after attachment to the uterine wall.
For a full comparison:
Blastocyst vs Embryo: Key Differences
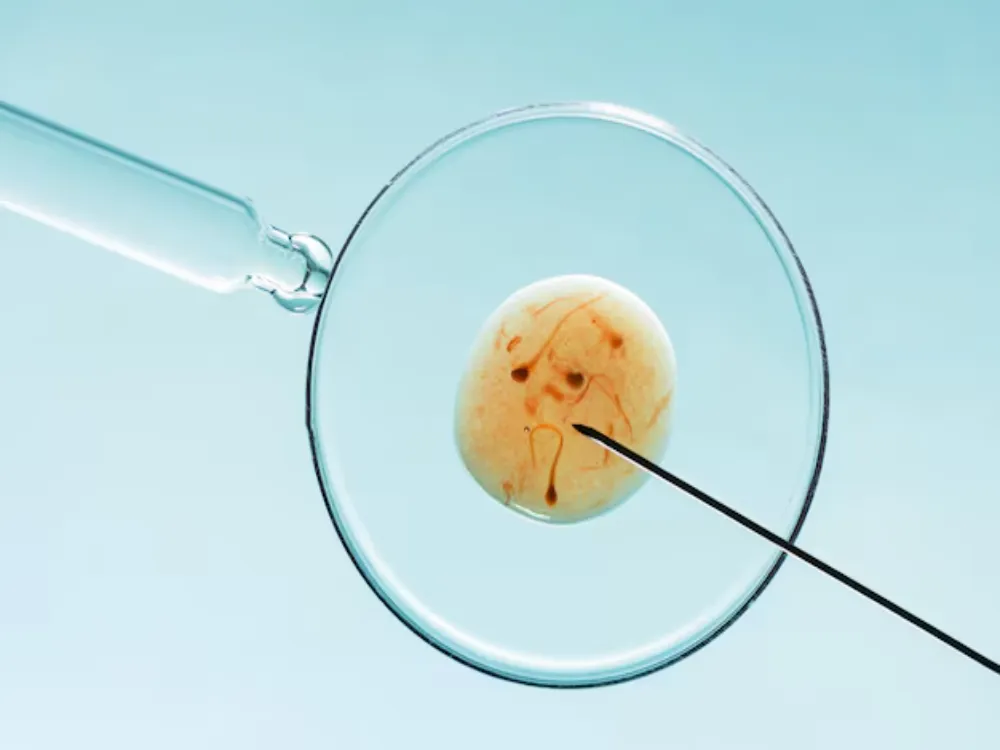
The question “What percentage make it to blastocyst?” is one of the most searched topics in IVF.

This approach does not remove risk—itrepositions risk earlier, allowing families to plan next steps with better information.
| Feature | Day-5 | Day-6 |
| Development speed | Faster | Slightly slower |
| Fresh transfer | Ideal | Less common |
| Frozen transfer | Excellent | Excellent |
| Euploid rate | Slightly higher | Slightly lower |
The question “What percentage make it to blastocyst?” is one of the most searched topics in IVF.
This typically occurs between Day 6 and Day 10.
Blastocysts are graded based on:
Expansion (1–6)
Indicates how expanded or hatched the embryo is.
ICM Grade (A/B/C)
Quality of inner cell mass.
TE Grade (A/B/C)
Quality of outer cell layer.
Example:
Higher grades suggest stronger implantation potential but do not guarantee pregnancy.
For detailed grading:

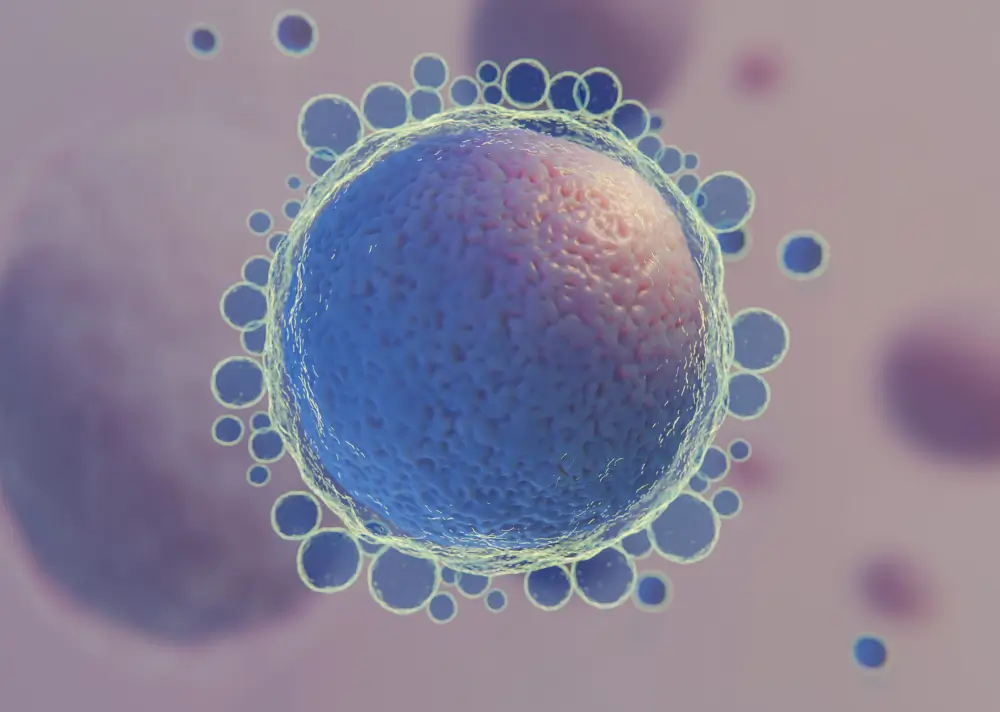
Genetic testing (PGT-A) is typically performed at the blastocyst stage.
A small sample of trophectoderm cells is removed and analyzed for chromosomal normalcy.
Benefits:
For detailed workflow:
| Stage | Key Feature |
| Zygote | Single cell |
| Morula | Compact ball |
| Blastocyst | ICM + TE + cavity |
| Gastrula | Germ layer formation |
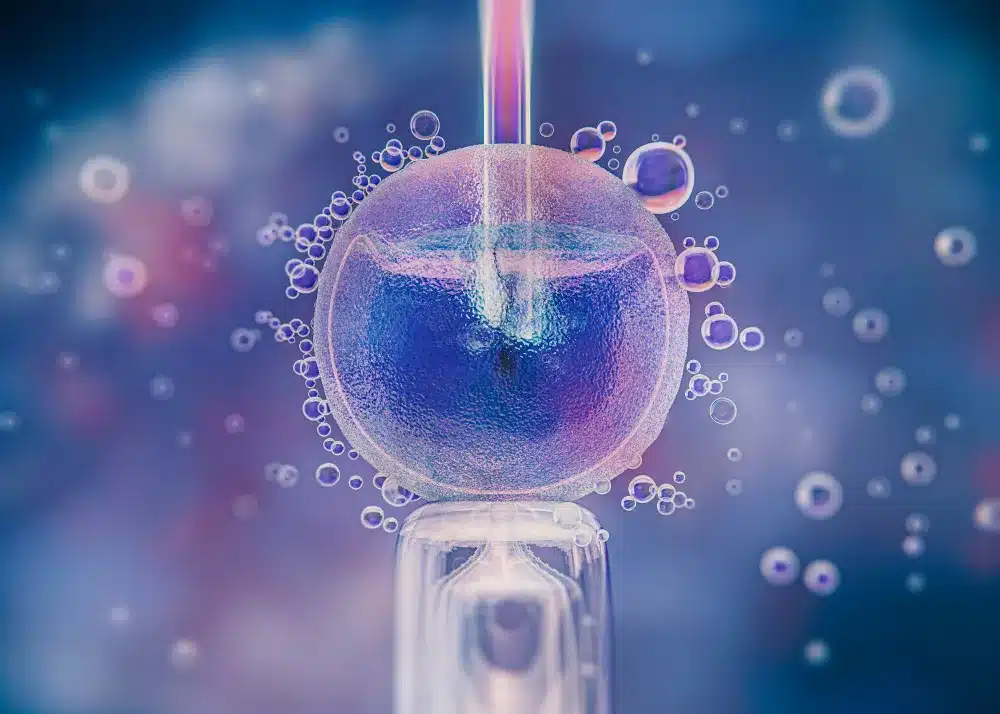
One of the most challenging aspects of IVF is uncertainty.
Families often begin treatment without knowing:
Guaranteed Blastocyst programs were developed to address this uncertainty.
Instead of starting with eggs and hoping embryos develop, these structured programs focus on achieving a defined minimum number of blastocysts before transfer planning begins.
“Guaranteed” refers to embryo quantity — not pregnancy.
Programs typically include:
EggDonors4All coordinates these programs.
All laboratory procedures are performed by licensed clinics.

Common reasons:
This approach does not eliminate risk.
It repositions risk earlier in the process.

For surrogacy journeys, embryo readiness affects:
Having defined blastocysts available allows structured coordination.
Related:
Searches for “blastocyst cost” often reflect desire for predictability rather than lower pricing.
Cost reflects:
Learn more:
For surrogacy journeys, embryo readiness often affects legal contracts, matching timelines, and coordination. Guaranteed blastocysts allow embryos to be prepared before surrogate matching begins.
For international families, this structure can reduce unnecessary travel and scheduling challenges by allowing much of the process to be coordinated remotely.
A Day-5 or Day-6 embryo with differentiated inner and outer cells.
About 40–60% on average.
Yes. Many Day-6 embryos implant successfully.
After implantation and gastrulation begin.
No. It refers only to embryo quantity.
Predictable outcomes. Transparent planning. Begin with confidence.
EggDonors4All provides education and coordination support only.
The blastocyst stage represents one of the most important biological milestones in IVF.
Understanding it allows families to:
For a structured, defined embryo approach:
Explore Guaranteed Blastocysts
Predictable outcomes. Transparent planning. Begin with confidence.
| Feature | Day-5 | Day-6 |
| Development Speed | Faster | Slower |
| Use | Fresh or frozen transfers | Mostly frozen |
| Grading | Often higher | More variable |
| Pregnancy Rates | Comparable when frozen |
Donor eggs often generate stronger embryo cohorts because:

EggDonors4All does not perform medical procedures. Partner fertility clinics handle all embryo creation, culture, and transfer.
A Guaranteed Blastocyst Program provides:
Having defined blastocysts available allows structured coordination.
Related:
This option often benefits families navigating:
Learn more:
No. Typically 30–50% reach Day-5 or Day-6.
No. It describes structure only.
Not necessarily—when frozen, outcomes are similar to Day-5.
Yes. Many successful pregnancies come from BB or BC grades.
Often, but depends on embryo cohort size and clinic strategy.
Only when intended parents choose PGT-A through their clinic.
No. All procedures are performed exclusively by licensed fertility clinics.
Yes—frozen blastocysts are commonly used in surrogacy cycles.
Predictable outcomes. Transparent planning. Begin with confidence.

Egg donation is a process where a woman (the egg donor) provides one or several eggs (also known as oocytes) for purposes of assisted reproduction, with the eggs being fertilized in the laboratory. Once fertilized, the resulting embryos are transferred to the recipient’s uterus to initiate a pregnancy, or they can be cryopreserved (frozen) for future use.